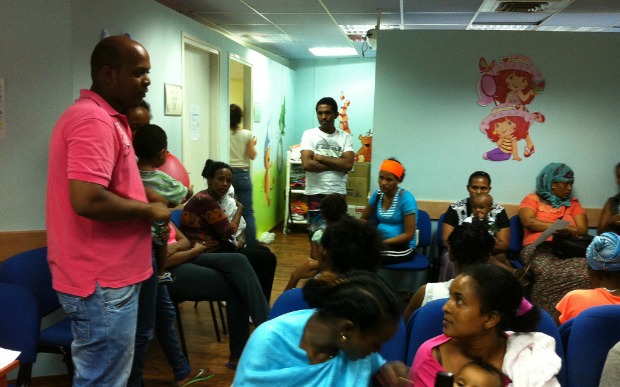An Israeli university graduate has founded a voluntary initiative to provide better and less costly healthcare to the approximately 60,000 Sudanese and Eritrean asylum-seekers and migrant workers living in Israel – two-thirds of them in Tel Aviv.
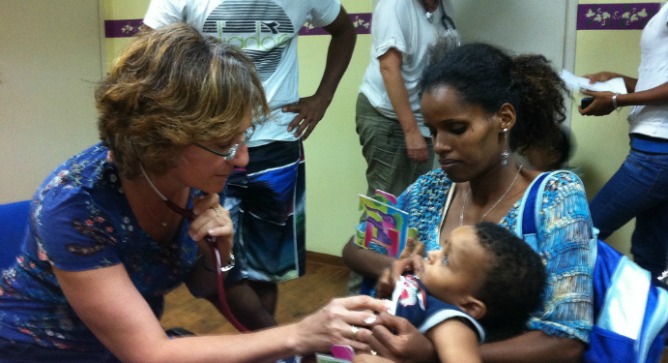
Based at the Israeli Ministry of Health’s clinic for refugees at the Tel Aviv Central Bus Station, Dr. Jonah Mink’s MigrantHealth:IL works to increase patient awareness of available resources and improve health literacy; overcome language and cultural barriers; coordinate care between providers; ensure follow-up; and reduce the overwhelming demand on local hospitals and clinics.
Spread the Word
• Email this article to friends or colleagues
• Share this article on Facebook or Twitter
• Write about and link to this article on your blog
• Local relevancy? Send this article to your local press
Mink, who graduated this year from Ben-Gurion University of the Negev’s Medical School for International Health, believes his organization, MigrantHealth:IL, “leverages the entrepreneurial spirit of Israel” to create more efficient solutions.
His ultimate goal is to share the model with other countries facing similar challenges related to global migration.
The program set up by Mink focuses on recruiting nurses from the migrant community who are fluent in either English or Hebrew, and establishing a decentralized electronic medical records database in cooperation with BGU’s School of Information Systems Engineering and the OpenMRS (Open Medical Records System platform) community.
“Those are our two flagship programs that will set the tone,” says Mink. “Our operating model is figuring out low-cost solutions that have great impact, getting them functioning well and then spinning them off to responsible bodies” to oversee for the long run.
WHO to market the model
Along with Tel Aviv Refugee Clinic director Orel Ben Ari and BGU medical student Tobin Greensweig, designer of the electronic medical record system now in place at the Village Health Works clinic in Burundi, Africa, Mink launched an Indiegogo crowd-funding campaign to raise $15,000 for MigrantHealth:IL. The Schusterman Family Foundation’s ROI Community promised to match the funds.
“This is the amount we need to run a six-month pilot program with nurses, and then spin it off after demonstrating how much time, energy and money we are saving,” says Mink.
Once it is proven in practice, a full package of processes, systems and tools will be marketed to other countries through the World Health Organization (WHO).
“We’re taking all the Israeli technology and innovation and bringing it to developed countries in Europe and North America that really don’t have effective and cost-effective systems for understanding and managing large cohorts of people from developing countries and integrating them into the mainstream health system,” Mink explains.
After the initial grant-funded pilot, the financial involvement of hospitals and the Israeli Health Ministry will allow for scaling and sustainability of MigrantHealth:IL.
“I know it’s going to work because I did it before in New York with community health programs [Millennium Villages Project and City Health Works], running with the same model to reduce unnecessary emergency room visits,” Mink says confidently.
Translation, triage and training
Nurses from the migrant communities, strategically placed at common contact points including the Tel Aviv Refugee Clinic, offer translation, triage, care coordination and health education. Mink says their efforts save Israeli hospitals money by decreasing repeat emergency visits, while also decreasing the burden on the clinic by improving the migrants’ overall health picture.
Mink relates how one of the volunteer nurses, an Eritrean man, extemporaneously gave a lesson on the importance of vitamin D to a group of African mothers and children waiting at the Tel Aviv clinic. “They are the most brilliant, motivated people I have ever met,” he says of these foreign-trained community health workers.
Implementing an electronic medical records system will help the clinic’s staff better manage care. Soon the database will be rolled out nationally to other clinics, hospitals and community organizations to integrate the gathering of patient information and care delivery for this population, Mink says.
He began working with the migrant population during his clinical rotation at the Tel Aviv Refugee Clinic last February. The Buffalo, New York native will return to the United States next year to begin a family medicine residency, and is passionate about improving efficiency in the delivery of medical care to marginalized communities.
“The coolest thing is that we are harnessing the spirit of Israeli innovation and entrepreneurship and applying it to the health needs of the most marginalized communities,” says Mink. “It’s not just about innovation, but innovation for the greater good — demonstrating how well it works and teaching the world how to do it well.”